Published on April 7 2026 In Research
Tuberculosis Outbreak in Nunavik | How Can We End the Tuberculosis Outbreak in Nunavik?
Tuberculosis remains a persistent public health challenge in Nunavik. In 2025, the region crossed an alarming threshold, recording a record number of active cases. A study published in the Canadian Medical Association Journal examines this concerning situation. Among its authors are two close collaborators of the INQ: Glenda Sandy, a Naskapi-Cree nursing consultant at the RRSSSN, and Faiz Ahmad Khan, holder of the INQ–McGill Northern Research Chair on the Optimization of Respiratory Health Services.
A methodology centered on self-determination
For the study’s authors, it was imperative that the research not be merely a data collection exercise, but an act of reconciliation in itself. The team, composed largely of Inuit and Indigenous researchers, used a participatory community research framework based on the values of respect, relevance, reciprocity, and accountability.
Under the guidance of the Puvaqatsianirmut Committee (Committee for Healthy Lungs), the researchers collected testimonies from 156 Inuit participants. This approach allowed the team to conclude that the current healthcare system fails to meet the population’s basic needs due to chronic underfunding and a shortage of resources.
The researchers' finding: a challenging system
The researchers’ findings describe a model of care that they characterize as program-centered. According to the team’s analysis, this paradigm forces Inuit patients to adapt to services limited by a lack of resources, rather than tailoring care to the individual. The authors identify several sources of significant suffering resulting from this model:
- Forced travel outside communities for examinations or isolation, which breaks family ties and compromises confidentiality.
- A loss of autonomy exacerbated by the mandatory nature of treatments and the threat of police or legal intervention.
- The near-total absence of Inuktitut, the patients’ mother tongue, in healthcare settings.
The team's vision: seven calls to action
Drawing on the expertise of Inuit participants (Nunavimmiut), the researchers formulated seven concrete calls to action to transform tuberculosis care in Nunavik. These recommendations aim to shift from a program-centered model to a person-centered model led by the Inuit.
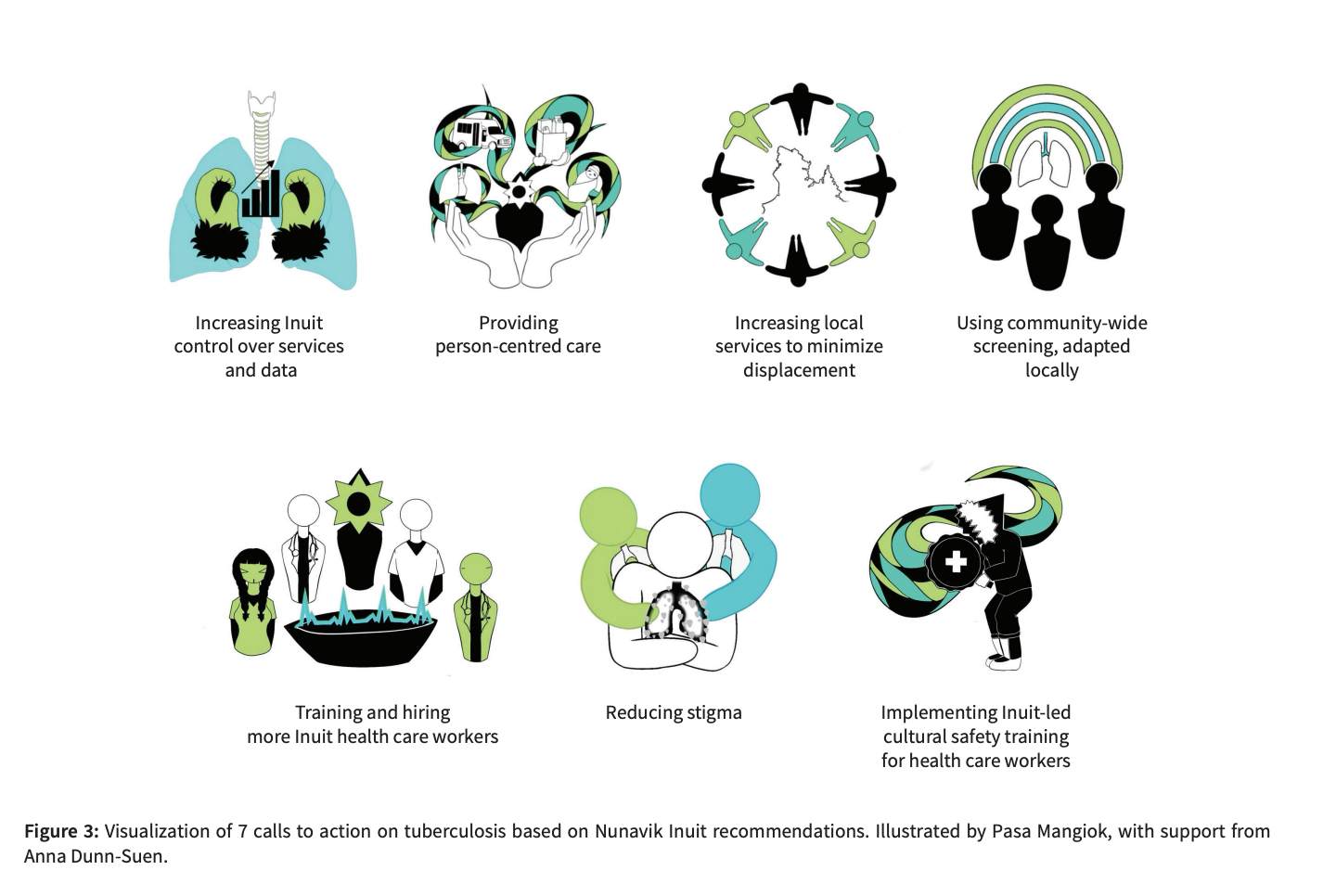
Calls to Action:
- Increase Inuit control over services and data: The community should lead efforts to prevent and eliminate the disease. Statistics must be used as real-time tools to inform local leaders of the exact situation in their village.
- Provide person-centered care: This involves offering practical support to reduce the burden on patients, such as transportation (a clinic bus), home delivery of medications, food vouchers, or childcare services to facilitate treatment adherence.
- Expand local services to minimize travel: Participants recommend establishing “tuberculosis centers” within the communities themselves and ensuring permanent access to X-ray services to prevent patients from being flown to regional hospitals or to the south.
- Use community-wide, locally adapted screening: “Door-to-door” screening is preferred to reach everyone, as not everyone listens to the radio. Universal screening also reduces suspicion and gossip by not targeting only certain individuals.
- Train and hire more Inuit healthcare workers: Having Inuit staff on hand would improve communication in Inuktitut and build trust. This would enable more culturally respectful care and could prevent the need to involve the police or the courts to enforce treatment.
- Reduce stigma: The focus should be on encouraging patients rather than blaming them. Researchers suggest disseminating clear information throughout the community to normalize the disease and eliminate the shame associated with infection.
- Implement Inuit-led cultural safety training for healthcare workers: Non-Inuit doctors and nurses must receive appropriate orientation on local values before arriving in Nunavik. Participants also call for greater staff stability to ensure continuity of care.
In conclusion, the study’s authors assert that the elimination of tuberculosis by 2030 can only be achieved if the governments of Quebec and Canada respond urgently to these calls. For the research team, it is imperative to move beyond mere acknowledgment to political action grounded in decolonization and Inuit self-determination.
See also:
Geboe, B., Sandy, G., Tooktoo, D., Tukalak, S., Law, S., White-Dupuis, S., Nappaaluk, Q., Aliqu, N., Quananack, E., Emudluk, M., Watt, L., Mangiok, P., Dunn-Suen, A., Yaaka, M., MacDonald, N. I., & Khan, F. A. (2026). Inuit experiences of and expertise on the 21st-century tuberculosis epidemic in Nunavik, Quebec: a qualitative community-based participatory study. CMAJ, 198(13), E474-E485. https://doi.org/10.1503/cmaj.251824
Orr, P. H. (2026). Promoting reconciliation through research. CMAJ, 198(13), E508-E509. https://doi.org/10.1503/cmaj.260331
Media coverage:
Desautels, K. (2026, 6 April). Comment venir à bout de l’épidémie de tuberculose au Nunavik ? La Presse. https://www.lapresse.ca/actualites/sante/2026-04-06/etude/comment-venir-a-bout-de-l-epidemie-de-tuberculose-au-nunavik.php
Lévesque, F. (2026, 6 April). Épidémie de tuberculose au Nunavik : les Inuit réclament un virage majeur. ICI Radio-Canada. https://ici.radio-canada.ca/nouvelle/2243998/epidemie-tuberculose-nunavik
Back to news

